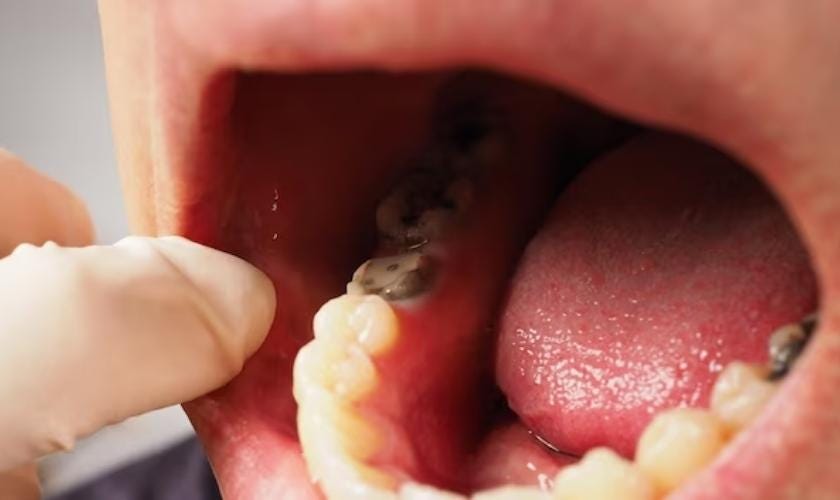
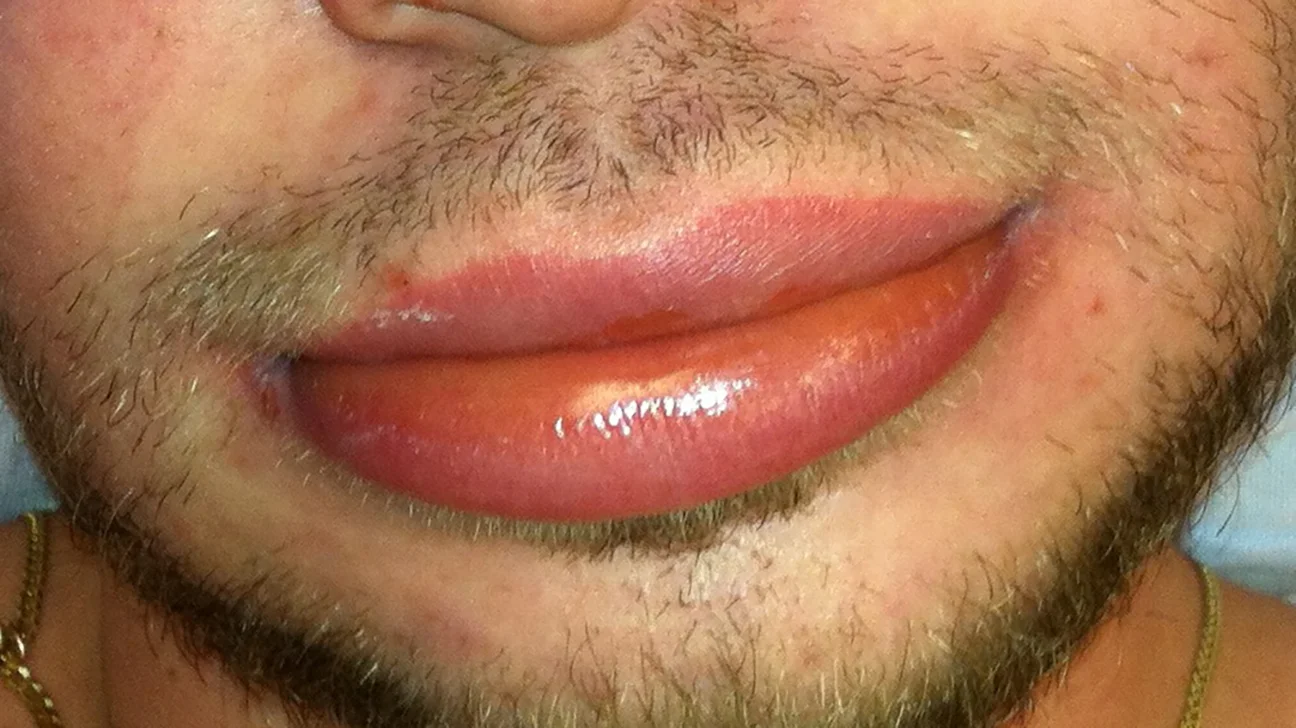
After taking antibiotics for a tooth infection, it usually takes 1 to 2 days to see improvement. It’s important to finish all the medicine to make sure the infection is completely gone.
If you don’t take the antibiotics like your doctor says or if the main problem causing the infection isn’t fixed, the infection might come back.
Sometimes, bacteria can become resistant to the antibiotics, making it harder to treat. To prevent the infection from returning, follow the dentist’s advice, keep your teeth clean, and go for regular check-ups. If your symptoms continue, it’s important to see the dentist again.
What is The Role of antibiotics in treating tooth infections?
Antibiotics serve as powerful weapons in the battle against tooth infections. When a tooth becomes infected, harmful bacteria multiply and cause pain, swelling, and other discomforts.
The role of antibiotics is to intervene and target these bacteria, hindering their ability to thrive and spread. By doing so, antibiotics help the body’s natural defense mechanisms to gain the upper hand in combating the infection.
They act as reinforcements, providing an extra line of defense to support the immune system in its fight against the invading bacteria.
How antibiotics work to combat bacterial infections
Antibiotics operate through various mechanisms to tackle bacterial infections. One common method involves disrupting the bacteria’s cell walls, preventing them from maintaining their structural integrity.
This weakens the bacteria, making it more susceptible to the body’s immune responses. Another approach is inhibiting the bacteria’s ability to produce essential proteins needed for their survival and reproduction.
By interfering with these vital processes, antibiotics effectively cripple the bacteria, halting their spread and causing them to die off.
What Are The Factors influencing the speed of recovery?
Type of Antibiotic: Different antibiotics have varying rates of absorption and action. Some act quickly, while others may take a bit longer to show noticeable effects.
Severity of Infection: The extent and severity of the infection play a significant role. In cases of mild infections, improvements may be observed sooner compared to more severe cases.
Individual Health: The overall health and immune system of the individual can influence how quickly antibiotics work. A robust immune system may enhance the antibiotic’s effectiveness.
Adherence to Prescription: Taking antibiotics as prescribed, including the correct dosage and completing the full course, is crucial for optimal effectiveness. Skipping doses or stopping treatment prematurely can hinder recovery.
Bacterial Resistance: In some cases, bacteria may develop resistance to certain antibiotics, affecting their efficacy. This emphasizes the importance of accurate diagnosis and prescription by healthcare professionals.
Underlying Health Conditions: Pre-existing health conditions can impact the body’s ability to respond to antibiotics. Conditions such as diabetes or compromised immune systems may prolong the recovery process.
What are the Signs of Improvement During Antibiotic Treatment?
Signs of improvement during antibiotic treatment for a tooth infection may become noticeable as the medication begins to take effect. While individual responses can vary, here are common signs that indicate the antibiotics are working:
Reduced Pain
One of the early signs of improvement is a decrease in toothache or pain associated with the infection. As the antibiotics combat the bacteria causing the infection, the discomfort should gradually lessen.
Decreased Swelling
Antibiotics help reduce inflammation, which is often a significant source of swelling around the affected tooth or gums. Improvement in swelling is a positive indication that the antibiotics are addressing the infection.
Lowered Temperature
In some cases, a tooth infection can cause a mild fever. As the antibiotics work to eliminate the infection, the body’s temperature may return to normal, signaling a positive response to treatment.
Improved Redness
If the gums or surrounding tissues were red and irritated due to the infection, a positive sign of improvement is a reduction in redness. This suggests that the inflammatory response is subsiding.
Enhanced Function
As the infection is brought under control, normal oral functions such as chewing and speaking should become less painful and more comfortable.
Improved Sleep
If the tooth infection was causing discomfort that affected sleep, an improvement in sleep quality can be an indication of the antibiotics working to alleviate pain and inflammation.
Overall Well-being
A general improvement in the individual’s well-being, energy levels, and mood may occur as the body responds positively to antibiotic treatment.
It’s important to note that while these signs suggest improvement, it’s crucial to complete the full course of antibiotics as prescribed by the healthcare provider.
Even if symptoms improve, stopping the medication prematurely can allow remaining bacteria to survive and potentially lead to a recurrence of the infection.
What Are The Potential Reasons for Tooth Infection Recurrence?
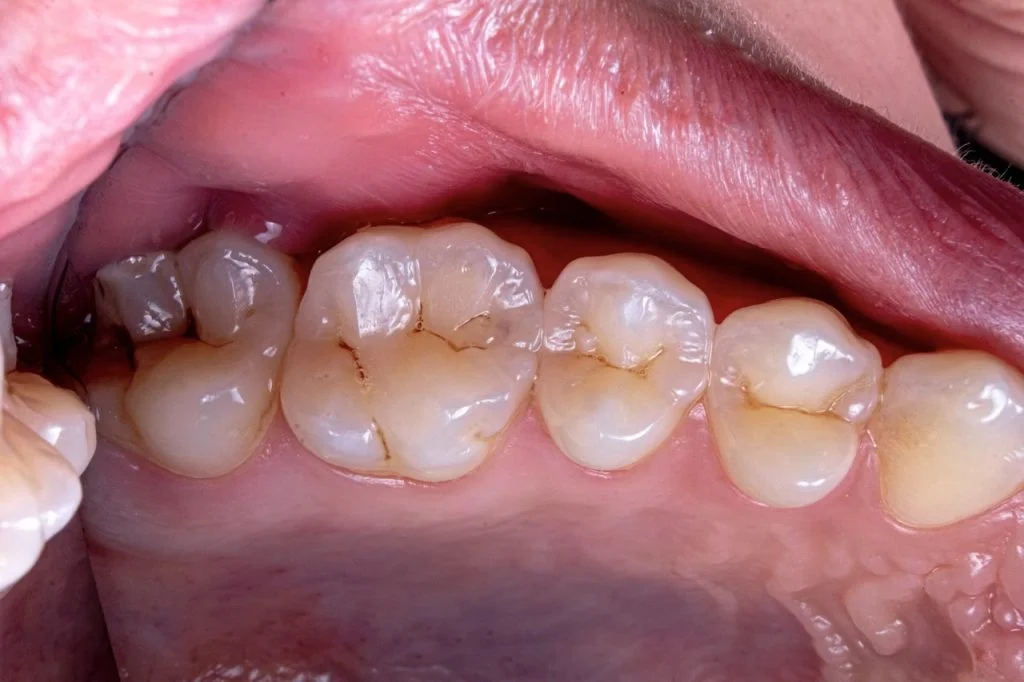
Incomplete Antibiotic Course
Incomplete antibiotic courses are a common reason for tooth infection recurrence. When a prescribed antibiotic course is not finished, there’s a risk that some bacteria may survive, leading to the development of antibiotic-resistant strains.
These surviving bacteria can cause a resurgence of the infection, potentially with increased resistance to the same antibiotic.
Individuals must adhere to the prescribed dosage and complete the entire course, even if symptoms improve before finishing the antibiotics.
Antibiotic Resistance
Antibiotic resistance occurs when bacteria evolve and develop mechanisms to withstand the effects of antibiotics. This can happen if antibiotics are overused or misused.
In the context of tooth infections, if antibiotics are repeatedly used without proper guidance or if the full course is not completed, bacteria may adapt and become resistant.
When this occurs, the effectiveness of previously effective antibiotics diminishes, making it more challenging to treat infections.
To mitigate antibiotic resistance, healthcare providers must accurately diagnose infections and prescribe antibiotics judiciously.
Reinfection from Untreated Causes
Addressing the root cause of a tooth infection is crucial to preventing recurrence. If the initial infection is not fully treated or if underlying issues such as dental decay, gum disease, or an abscess are not resolved, there’s a risk of reinfection.
For example, if a cavity is not properly filled or if gum disease persists, bacteria can multiply, leading to another infection.
Comprehensive dental care, including addressing the underlying causes of the initial infection, is essential to prevent recurrence and promote long-term oral health.
How Long Before a Tooth Infection Comes Back?
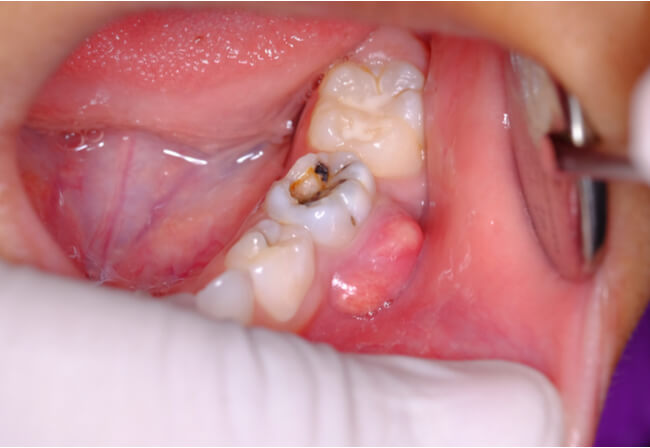
The time it takes for a tooth infection to come back varies and depends on several factors. There is no fixed timeline, and individual experiences can differ. Some key factors influencing the potential recurrence of a tooth infection include
Completing Antibiotic Course
If an antibiotic course is not completed as prescribed, it increases the risk of the infection returning. It’s crucial to finish the entire course to ensure all bacteria are eliminated.
Severity of Infection
The severity of the initial infection plays a role. More severe infections may take longer to completely resolve, and there might be a higher risk of recurrence if the infection was not fully treated.
Underlying Dental Issues
If the root cause of the infection, such as untreated dental decay or gum disease, is not addressed, there’s a higher likelihood of the infection returning. Comprehensive dental care is essential to prevent recurrence.
Antibiotic Resistance
If bacteria develop resistance to the prescribed antibiotics, the infection may return. Proper diagnosis and appropriate antibiotic selection are crucial to avoid resistance.
Individual Immune Response
The effectiveness of the immune system in combating the infection also influences the likelihood of recurrence. A strong immune response can aid in preventing the return of the infection.
Tips for Preventing Tooth Infection Recurrence
Importance of Good Oral Hygiene
Maintaining good oral hygiene is paramount in preventing tooth infection recurrence. Brush your teeth at least twice a day using fluoride toothpaste to remove plaque and bacteria.
Floss daily to clean between teeth and along the gumline, where a toothbrush may not reach. This routine helps prevent the buildup of harmful bacteria and reduces the risk of infections.
Regular Dental Check-ups
Regular dental check-ups are a crucial part of preventive care. Schedule routine visits with your dentist, typically every six months, to monitor your oral health.
Professional cleanings and examinations allow dentists to identify potential issues early on, address concerns, and provide personalized advice to prevent the recurrence of tooth infections.
Following Post-Treatment Care Guidelines
After receiving dental treatment, whether for an infection or another issue, following post-treatment care guidelines is essential. Your dentist will provide specific instructions on how to care for your teeth and gums during the recovery period.
When to Seek Professional Help Again
If you have persistent tooth pain, swelling, difficulty chewing, or changes in tooth color, it’s time to see your dentist. Ignoring these symptoms may lead to more significant problems, so seek professional help promptly for early intervention and effective dental care.
Signs Indicating the Need for Further Dental Consultation
Recognizing signs that warrant further dental consultation is crucial for maintaining oral health. If you experience any of the following, it’s advisable to seek professional help
If you continue to experience persistent or worsening tooth pain, it may indicate an ongoing issue that requires attention.
Swelling around the gums, face, or the presence of pus near the affected tooth can be signs of an unresolved infection or abscess.
If you encounter difficulties while chewing or biting, it may indicate problems with the affected tooth or surrounding structures.
Increased sensitivity to hot or cold substances, especially after a dental procedure, may signal an underlying problem.
Any noticeable changes in the color of the affected tooth may suggest complications that need professional evaluation.
Importance of Not Ignoring Symptoms:
Ignoring dental symptoms can lead to the exacerbation of problems and increase the risk of complications.
It’s essential not to dismiss signs of discomfort, pain, or changes in oral health. Ignoring symptoms may allow infections or other dental issues to progress, potentially leading to more extensive treatments or irreversible damage.
Early intervention is key to effective dental care. Seeking professional help promptly when symptoms arise allows dentists to diagnose and address issues in their early stages, often resulting in less invasive and more successful treatments.
Regular dental check-ups, even when no apparent issues are present, contribute to preventive care.
Dentists can identify potential concerns before they cause noticeable symptoms, emphasizing the importance of proactive dental healthcare.
FAQ
How many times can you take antibiotics for a tooth infection?
The number of times you can take antibiotics for a tooth infection depends on the severity and recurrence of the infection. It’s crucial to follow your dentist’s guidance, and they will determine the appropriate course of treatment based on your specific situation.
Can an infection come back after antibiotics?
Yes, an infection can return after antibiotics if the prescribed course is not completed, the root cause is not addressed, or if antibiotic-resistant bacteria develop. Following the full antibiotic course and addressing the underlying dental issues are essential to prevent recurrence.
How do you know if antibiotics are not working for a tooth infection?
If your symptoms persist or worsen despite taking antibiotics, it may indicate that they are not effective. In such cases, consult your dentist promptly for a reevaluation and adjustment of the treatment plan.
What if my tooth still hurts after antibiotics?
If tooth pain persists after completing the antibiotic course, it suggests the infection may not be fully resolved. Contact your dentist to determine the cause, as further evaluation and additional treatment may be necessary.
What is the strongest antibiotic for a tooth infection?
The choice of antibiotic depends on the specific bacteria causing the infection. Amoxicillin is commonly prescribed, but your dentist will determine the most suitable antibiotic based on the type of infection and your medical history.
Is 5 days of antibiotics enough for a tooth infection?
The duration of antibiotic treatment varies, and 5 days may be sufficient for certain cases. However, your dentist will decide the appropriate length based on the severity of the infection and the specific antibiotic prescribed.
Do antibiotics always cure tooth infections?
While antibiotics can effectively treat tooth infections, they may not address the root cause. Comprehensive dental care, including addressing underlying issues, is essential for long-term success.
Can antibiotics heal an infected root canal?
Antibiotics can help control infection but may not fully heal an infected root canal. A root canal procedure is often necessary to remove infected tissue and save the tooth. Consult your dentist for personalized advice.
Final thoughts
On the whole, completing the full antibiotic course, tackling the root cause, and keeping up with good oral care are key in avoiding a tooth infection comeback. If problems persist, don’t hesitate to reach out to your dentist for ongoing support in maintaining oral health.